A comparison of 16 major cross-disorder mental health assessment tools shows that none provide a complete picture of a patient’s mental health symptom profile. The Mental Health Quotient or MHQ fills this gap.
In previous posts we’ve talked about the ambiguous nature of disorder definitions (see Quantitative Similarity of Depression Tools and The Ambiguous Symptoms of Autism). This results in a challenge for research attempting to link disorders to biological underpinnings and begs the need for a cross-disorder or disorder agnostic symptom inventory. Here we look at the cross-disorder inventories available today.
See EEG Based Biomarkers and the Many Pitfalls
Using an analysis of 112 widely used assessment tools across all major mental health disorders we found that they encompassed 170 symptoms which could be combined into 43 major symptom categories. We then looked at each of 16 different cross-disorder assessment tools (9 adult, 7 pediatric) in terms of the breadth of symptoms that they assess, as well as the similarities and differences between them. To do this we coded each question by both symptom category as well as symptom “theme” – whether it referred to an emotion, cognition or behavior or a trigger or consequence of these.
16 Cross Disorder Tools
Here is a list of the questionnaires and interviews we looked at. Some are formatted as a list of symptoms spanning multiple disorders (e.g. Symptom Checklist 90; Child Behavior Checklist), while others are organized into disorder specific modules (e.g. Kiddie Schedule for Affective Disorders and Schizophrenia; Structured Clinical Interview for DSM-5). These tools are commonly used to either screen for, or diagnose psychiatric disorders in clinical practice, or in research studies aiming to develop new clinical biomarkers.
| Adult | Children/Adolescents |
| APA DSM–5 Self-Rated Level 1 Cross-Cutting Symptom Measure (APA-CC-A) | APA DSM–5 Self-Rated Level 1 Cross-Cutting Symptom Measure (APA-CC-C) |
| Brief Symptom Inventory (BSI) | Child behaviour Checklist (CBC) |
| WHO Composite International Diagnostic Interview, Computer Assisted Personal Interview, Version 21.1.4 (CIDI CAPI) | Diagnostic Interview Schedule for Children (DISC-IV) |
| Kessler Psychological Distress Scale (K10+) | Kiddie Schedule for Affective Disorders and Schizophrenia, Lifetime Version, DSM-5 (KSADS-PL-5) |
| Mini International Neuropsychiatric Interview (MINI) | PROMIS Profile 49 (PROMIS-Profile-C,) |
| PROMIS Profile 57 (PROMIS-Profile-A) | PROMIS Question Bank (PROMIS-QB-C) |
| PROMIS Question Bank (PROMIS-QB-A) | Strengths and Difficulties Scale (SDS) |
| Structured Clinical Interview for DSM-5 – Clinical version (SCID-5-CV) | |
| Symptom Checklist 90 Revised (SCL-90-R) |
Coverage of the breadth of mental health symptoms.
How well did these tools cover all 43 symptom categories? When we looked across all 16 assessment tools combined, then they did indeed assess all 43 symptoms. However, when we looked at each tool individually, the maximum percentage of symptoms covered by any single cross-disorder tool was 86% (for the Structured Clinical Interview for DSM-5) indicating that none of the tools we looked at covered the full breadth of these 43 psychiatric symptoms. Moreover, only 9 of these 43 symptoms were assessed by 80% or more of the cross-disorder assessment tools – these were Attention & Concentration & Mental Focus; Energy Levels; Pains & Aches; Attachment & Affiliation; Confidence & Self Judgement; Anger & Irritability; Fear, Panic & Anxiety; Mood & Outlook and Interest, Effort & Motivation – illustrating the substantial heterogeneity and gaps across tools.
What themes do they cover?
In terms of symptom themes, we found that the cross-disorder tools were also biased in terms of their symptom theme assessments. For instance, the Brief Symptom Inventory and Kessler Psychological Distress Scale were primarily focused on asking about emotional symptoms (78% and 63% respectively) while others, such as the Child Behavior Checklist and Strengths and Difficulties Scale, were more heavily weighted towards asking about behavioral symptoms (47% and 50% respectively). These differences can be explained to some degree by the split between adult and pediatric tools, where, in general, the adult tools more heavily focus on assessing the way the person feels and children are more likely to be assessed based on observed behaviors. However, it points to a fundamental difference in approach that likely has substantial ramifications.
Similarity across tools.
To determine the similarity between the cross disorder tools, we computed a symptom similarity score* between each pair of assessment tools. When looking across the 16 tools, the analysis showed that, on average, the cross-disorder tools were only 33% similar (ranging from 9% similar between BSI and K10+ to 63% similar between KSADS and DISC-IV) revealing the extent of the inconsistency across assessment tools. Thus each tool paints a distinct but incomplete picture of the patients symptom profile.
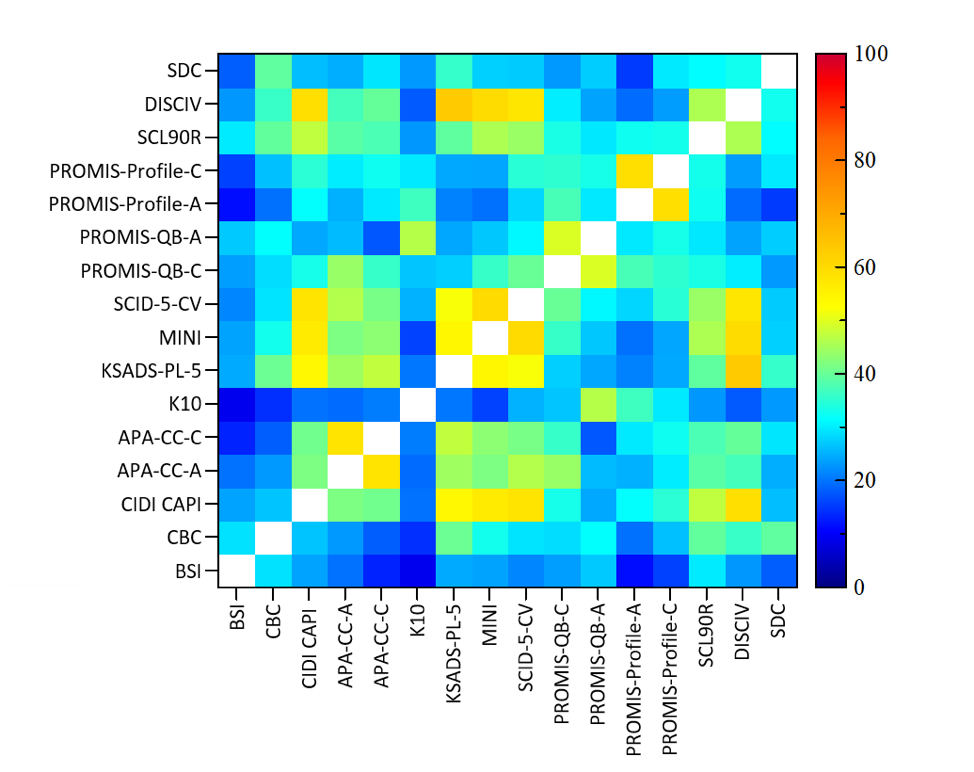 Color Matrix of Similarity Scores across Assessment Tools
Color Matrix of Similarity Scores across Assessment Tools
The consequence of all this is that it introduces variability, bias and inconsistency into clinical diagnosis and evaluation, further complicated by the fact that patient experience itself is highly heterogeneous.
See The Challenges of Mental Health Diagnosis
The MHQ: A new approach
To address this, Sapien Labs has developed a new assessment tool called the Mental Health Quotient (MHQ) which covers the complete breadth of mental health symptoms in a manner that is not based on any disorder classification or biased by any individual disorder (See Introducing the Mental Health Quotient). Its serves as a topline assessment of population mental health that is not tied to an arbitrary system of disorder classification that can both provide a view of population mental well being and identify at risk individuals based on complete symptom profiles.
Contribute to our “1 Million Project”.
If you would like to contribute to our research project which aims to map mental health and well being over a global population by collecting data from 1 million people spanning all countries of the world, then please click here to take the Mental Health Quotient Assessment. It takes ~15 minutes to complete and the data will ultimately be used to support the development of new platforms which promote positive mental health.
*Symptom similarity scores were first calculated as the min/max of the percentage of questions in each symptom category. We then computed a weighted average using the mean of the percentage of questions in each symptom category as the weighting factor to arrive at a questionnaire level similarity score. This meant that symptom level similarity scores were weighted more strongly when the symptom was associated with a greater proportion of questions.

Hi,
this sound as an innovative project, with important consequences for mental health assessment.
The phrasing of complaints may be different in various languages. Therefore, it would be interesting to assess these in other languages as well, and compare these in terms of structural equivalence. Also, apart from any norm group construction and cut-off scores, validation with mental health instruments that did not make part of the initial analyses is still required. Also other instruments, e.g., WHOQOL may serve well for validation. Again this may be different for various languages. Wishing you all the best!
Hi Rien, Many thanks for your comments and suggestions. Yes, we are planning to expand the MHQ into other languages in the near future to not only ensure it has a broad reach but also so we can make these kind of comparisons. As part of our initial phase of data collection and analysis, we’re doing work to validate the tool in various ways and the WHOQOL is a good suggestion.