Comorbid mental health disorders are the norm rather than the exception. When most people have multiple disorders, comprehensive symptom profiles are essential to understand the patient.
Amongst the many challenges facing the current system of mental health diagnosis, the vast comorbidity seen across patients – something that is more the norm than the exception [1,2] – is one that is clearly at odds with the categorical approach to disorder labelling. It is also something that we clearly see within the data generated by the Mental Health Million Project.
See related post 3 Challenges in Mental Health Assessment
In a previous post (How true are DSM disorder classifications to real-life symptom profiles?) we showed how, based on a dataset of 10,000, 81% of respondents with MHQ scores corresponding to the most severe “clinical” score level had symptom profiles that aligned with more than 1 disorder label.
Expanding this with an updated dataset of 25,000 respondents we find that, within the clinical MHQ score group, 82% have symptoms profiles that align with the criteria for more than 1 disorder, and within the “at risk” MHQ group, 42% have symptoms profiles that align with the criteria for at least 1 disorder and of these, 44% align with criteria for more than 1 disorder. With such a huge amount of disorder comorbidity exhibited by respondents who are experiencing the greatest challenges with their mental health, simply allocating a single disorder label to these individuals would likely be inappropriate and a poor reflection of their actual symptom experience.
The nature of comorbidities
Out of the 10 disorders that we map to within the MHQ (see [3] for more details about how this mapping is done), which disorders are most prevalent, and which comorbidities are most likely to occur?
Within the data collected from these 25,000 respondents, we looked at those who either had clinical or at risk MHQ scores whose symptom profiles aligned with at least 1 disorder to first see the prevalence for individual disorders. When we do this, we find that respondents are most likely to have symptom profiles that align with criteria for OCD (64%; (note that OCD criteria in this dataset does not distinguish obsessive thoughts from behaviors so may overestimate OCD incidence) and depression (47%) suggesting that within our current dataset, these disorder profiles are the most prevalent.
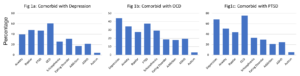
We then looked across pairs of disorders to see which disorders had the greatest comorbidity. We found that 72% of respondents whose symptom profiles aligned with depression criteria also aligned with generalized anxiety criteria, and 78% also aligned with eating disorder criteria. We also found that 80% of respondents whose symptom profiles aligned with addiction criteria also aligned with OCD criteria ; 86% respondents whose symptom profiles aligned with ADHD criteria also aligned with OCD criteria, while 86% of respondents whose symptom profiles aligned with OCD criteria also aligned with generalized anxiety criteria.
The need for a more transdiagnostic approach.
This preliminary pattern of comorbidities, which we will be better able to tease apart as the number of respondents from the Mental Health Million Project increases, adds further weight to the growing criticism of disorder criteria and categories that appear so at odds with evidence from real-life symptom profiles. The funneling of patients towards one diagnosis or another within the current diagnostic system forces clinicians to ignore or compensate for these comorbidities, even when they are in plain sight, encouraging them to instead take a best-fit approach that is suboptimal, and potentially skewing treatment decisions along the way.
See related post What are Mental Disorders?
To do justice to the real-life symptom profiles that people exhibit requires a more transdiagnostic approach where assessments can take into account the heterogeneity and diversity of symptoms and disorders that patients can exhibit, and where treatment decisions, and our understanding of the underlying biology, aren’t skewed by allocating people to single disorder categories.
See related post Taking a Transdiagnostic Approach to Mental Health Research
References
[1] Maj, M., ‘Psychiatric comorbidity’: an artefact of current diagnostic systems? British Journal of Psychiatry, 2005. 186(3): p. 182-184.
[2] Plana-Ripoll, O., et al., Exploring Comorbidity Within Mental Disorders Among a Danish National Population. JAMA Psychiatry, 2019. 76(3): p. 259-270.
[3] Newson, J., & Thiagarajan, T. (2020). Assessment of Population Well-Being With the Mental Health Quotient (MHQ): Development and Usability Study. JMIR Mental Health, 7(7), e17935. doi: 10.2196/17935