The many social, financial and health adversities caused by the Covid-19 pandemic have had a substantial impact on mental health.
The Covid-19 pandemic has touched all corners of the globe, causing illness, distress and uncertainty that is unrivalled in recent history. Although the primary objective of governments around the world has been to minimize serious illness and reduce death tolls, the policies put in place, such as social distancing, business closures and travel bans, have brought considerable social and financial fallouts that have secondary impacts on people’s livelihoods and mental wellbeing [1]. As part of the Mental Health Million project we’re specifically looking at the impact of the pandemic on people’s mental wellbeing to get a feel for which populations have been most affected and to see which impacts are taking the greatest toll.
An aggregate decline.
For an overall perspective of the impact of Covid-19, we compared data we collected in 2020 (n=~49,000) against a smaller subset of data that we collected in 2019 (n=~2000). In 2020, 26% of adults reported severe challenges (clinical or clinical risk) with their mental welling, up from 14% in 2019. This is also in line with what other researchers have been reporting [2-4], and mirrors reports of increasing numbers of people seeking help for mental health concerns, likely hindered by the disruption that there has been to the provision of care [5].
Social, financial and health adversities.
In our MHQ assessment, we’ve also asked people about various health, social and financial impacts and adversities that they have experienced due to the pandemic. We’ve then compared this against people’s mental wellbeing scores to get an indication of which ones might be taking the greatest toll on people’s mental wellbeing.
First, the data shows that 3.9% of respondents reported having had a Covid-19 infection of which 0.7% reported a severe case, roughly reflecting the global infection rate in 2020. On the other hand, a full 57% experienced a range of negative health, financial and/or social consequences. The 2% of respondents who were unable to get critical care for other existing health conditions due to the pandemic reported the poorest mental wellbeing. Their MHQ scores were, on average, 61 points lower along the scale (ranging from -100 to +200), which equates to a 20% decrease in mental wellbeing compared to those who had experienced none of the key listed consequences.
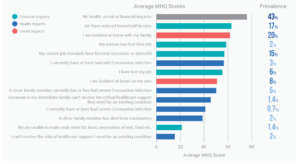
This decline is larger than what we see for the 0.7% who reported having had a severe case of Covid-19 (a decline of 35 MHQ points) or for the ~2% who lost a close family member to Covid-19 (a decline of 37 MHQ points). Further, it was the 1.4% of people who struggled to make ends meet for basic necessities who had the second lowest mental wellbeing, with scores on average 55 MHQ points lower than those who experienced none of the listed consequences.
On the other hand, the most widely experienced adversities were reduction household income (17% of our sample) and social isolation with family (20% of our sample), both of which were associated with a 13/14 point reduction in MHQ scores.
Differences across countries and age groups
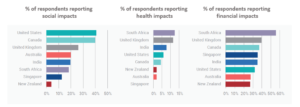
Countries have differed in their Covid policies as well as caseloads. It’s not surprising therefore that we see differences across countries. Of the eight countries surveyed, respondents from South Africa and the United Kingdom experienced the greatest health and financial impacts, whilst those in the United States and Canada saw the biggest impact with respect to social isolation. In contrast, the impact of Covid-19 was lowest for those in New Zealand and Singapore.
 There were also substantial differences across age groups. For example, for those aged 18-24, social isolation, with family or alone, had an enormous toll with mental wellbeing at 35% and 69% lower respectively compared to those who had no Covid-19 related adversities. In contrast, social isolation had a milder impact in those aged 65+ with mental wellbeing scores only 14-20% lower. On the other hand, severe issues such as not being able to make ends meet or being unable to receive critical care for a pre-existing condition had a dramatic toll on both age groups, while financial impacts had a greater toll in the 25-64 age group.
There were also substantial differences across age groups. For example, for those aged 18-24, social isolation, with family or alone, had an enormous toll with mental wellbeing at 35% and 69% lower respectively compared to those who had no Covid-19 related adversities. In contrast, social isolation had a milder impact in those aged 65+ with mental wellbeing scores only 14-20% lower. On the other hand, severe issues such as not being able to make ends meet or being unable to receive critical care for a pre-existing condition had a dramatic toll on both age groups, while financial impacts had a greater toll in the 25-64 age group.
See related post The Generational Decline In Mental Wellbeing
Access the Mental Health Million data
Data from the Mental Health Million project is openly available to the research community. Learn more and request access here to find deeper insights on this impact and the relationships between factors.
Read the Mental State of the World Report 2020
References
[1] Aknin, L. B., De Neve, J. E., Dunn, E. W., Fancourt, D., Goldberg, E., Helliwell, J., … Amor, Y. B. (2021, February 19). A Review and Response to the Early Mental Health and Neurological Consequences of the COVID-19 Pandemic. https://doi.org/10.31234/osf.io/zw93g
[2] Holmes, E.A., O’Connor, R.C., Perry, V.H., Tracey, I., Wessely, S., Arseneault, L., et al. (2020). Multidisciplinary research priorities for the COVID-19 pandemic: a call for action for mental health science. The Lancet Psychiatry 7(6), 547-560. doi: 10.1016/S2215-0366(20)30168-1.
[3] Pierce, M., Hope, H., Ford, T., Hatch, S., Hotopf, M., John, A., et al. (2020). Mental health before and during the COVID-19 pandemic: a longitudinal probability sample survey of the United Kingdom population. The Lancet Psychiatry 7(10), 883-892. doi: 10.1016/S2215-0366(20)30308-4.
[4] Serafini, G., Parmigiani, B., Amerio, A., Aguglia, A., Sher, L., and Amore, M. (2020). The psychological impact of COVID-19 on the mental health in the general population. QJM : monthly journal of the Association of Physicians 113(8), 531-537. doi: 10.1093/qjmed/hcaa201.
[5]https://www.who.int/news/item/05-10-2020-covid-19-disrupting-mental-health-services-in-most-countries-who-survey
[6] Turner, R.J., and Lloyd, D.A. (1995). Lifetime traumas and mental health: the significance of cumulative adversity. J Health Soc Behav 36(4), 360-376.


