The ‘diagnosis’ of Autism has a great deal of heterogeneity with a very different range of symptoms considered depending on the tools used.
The landscape of mental health assessment is typically organized around clusters of predefined symptom criteria which have been defined as specific mental health disorders. The diagnosis of a disorder therefore depends on disorder specific assessment tools that look for a set of symptoms.
See The Challenges of Mental Health Diagnosis
But within any one disorder, there are multiple assessment tools. Are these assessment tools roughly asking about the same set of symptoms? Or are there differences and inconsistencies in symptom assessment which could have implications from both a clinical and a research perspective? For example, if two research groups are searching for disorder-specific clinical biomarkers, but using different assessment tools which offer varying perspectives into the patient experience then where does this leave us when trying to compare and contrast their results?
See EEG Based Biomarkers and the Many Pitfalls
Review of assessment tools
In a previous post we talked about the range of tools which are used to assess depression (see 15 Depression Assessment Tools and Their Differences), and revealed that there is considerable heterogeneity in the symptoms that different depression scales and questionnaires ask about (see The Difficulty of Diagnosing Depression). But is this just the case for depression, or does it apply to other mental health disorders as well?
To explore this, we reviewed 15 subjective assessment tools which have been developed to screen for autism spectrum disorders [1]. As with the depression scales, we selected measures based on their citation number in the literature, and coded each question, within each questionnaire, based on the symptom(s) their asked about. We included 12 child/adolescent assessment tools which are parent or clinician reported, as well as 3 adult assessment tools which are self report or clinician reported.
Here is the list of assessment tools we looked at:
| Children/Adolescents | Adults |
| Social Communication Questionnaire (SCQ) | Autism spectrum quotient Adult 10 (AQ-Adult-10) |
| Gilliam Autism Rating Scale (GARS 3rd Edition) | Adult Asperger Assessment (AAA) |
| Childhood Autism Rating Scale (CARS, 2nd edition, standard version) | Broad Autism Phenotype Questionnaire (BAPQ) |
| Childhood Autism Rating Scale (CARS, 2nd edition, high functioning version) | |
| Social Responsiveness Scale (SRS, 2nd edition) | |
| Autism Spectrum Screening Questionnaire (ASSQ) | |
| Autism spectrum quotient Child 10 (AQ-Child-10) | |
| Autism spectrum quotient Adolescent 10 (AQ-Adolescent-10) | |
| Checklist for Autism in Toddlers (CHAT) | |
| M-Chat – Revised (2018 edition) (M-CHAT) | |
| The Childhood Autism Spectrum Test (CAST) | |
| Autism Diagnostic Interview-Revised (ADI-R) |
Pattern of symptom assessment
Based on an analysis of assessment tools from 9 different disorders (+120 tools in total), each question was coded as asking about a particular symptom category ranging from sleep, to flexibility, to fear and anxiety. Symptom categories were defined based on the linguistic meaning of the question and resulted in the identification of 43 unique symptom categories. By calculating the percentage of questions within each questionnaire that asked about each of these 43 symptoms categories we were able to look at the consistency or inconsistency in the symptoms that different autism spectrum disorder assessment tools ask about.
The results are shown in the figure below.
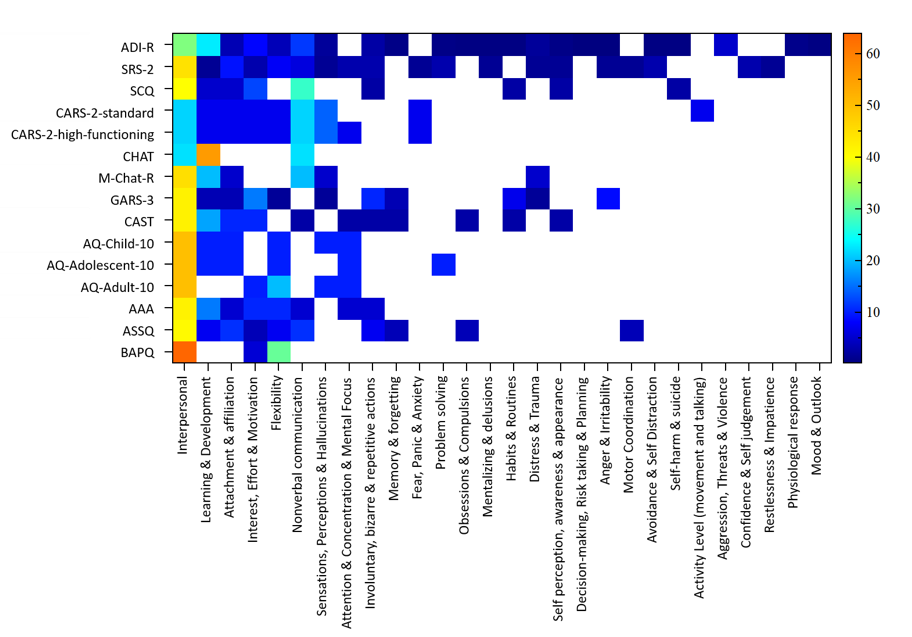 Figure1: Percentage of questions which asked about each symptom type for each assessment tool
Figure1: Percentage of questions which asked about each symptom type for each assessment tool
The plot shows that the most consistent symptom being asked about when assessing autism spectrum disorders is in relation to interpersonal experiences. This symptom category includes things like conversation skills, cooperation and joining in, social engagement and understanding, imitation, and speech and language and accounted for 25% to 50% of questions within each assessment tool. Many of the assessment tools (+70%) also ask about development, attachment, interest and flexibility. Beyond this, the remaining 50% to 70% of questions had a relatively heterogeneous pattern, where symptoms are asked about in some questionnaires, but not others. Furthermore, while a couple of Autism assessment tools (ADI-R and SRS-2) asked about a wide range of symptoms such as relating to mood and outlook and sleep, others assessed a relatively narrower range.
Thoughts, feelings and behaviors.
Another way to look at the data is by asking whether the questions assess the way people feel (emotion), the way they act (behavior), the way they think (cognitive), their physical symptoms (physical), or the consequences, triggers or treatment of the symptoms. When you look at the distribution of these themes across the different assessment tools then the data looks like this:
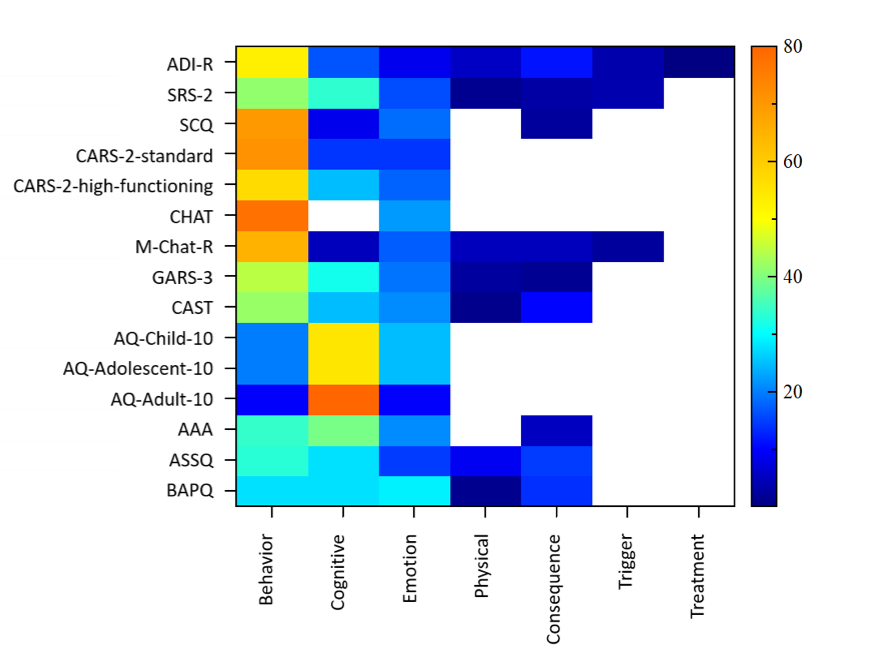 Figure2: Percentage of questions which focused on each symptom theme (e.g. emotion, cognitive, behavior) for each assessment tool
Figure2: Percentage of questions which focused on each symptom theme (e.g. emotion, cognitive, behavior) for each assessment tool
One finding from this plot is that, with the exception of the AQ questionnaires [2] which look more specifically at cognitive aspects, the majority of the assessment tools for child/adolescent populations primarily focus on the behavior of the individual. This is perhaps not that surprising given the rater for these tools is a parent, teacher or clinician rather than the individual themselves. But it also means that the assessment and diagnosis of autism spectrum disorders is predominantly being made on an interpretation and consideration of the way the person behaves, especially in a social context (as shown in figure 1) rather than the way they think or feel (see Autism and Individuality), which is in stark contrast to how depression is assessed (see 15 Depression Assessment Tools and Their Differences).
A disorder independent approach
Having assessment tools which are very disorder specific, obviously allows the clinician to deep dive into the specific pattern of symptoms which have been preassigned to that particular disorder, but it also runs the risk of skewing their perspective and not providing them with a complete picture of the symptoms that the person is experiencing. This assessment bias, as well as the heterogeneity across questionnaires, also has implications for research studies trying to identify reliable clinical biomarkers [e.g. 3,4].
As researchers aim to take a more transdiagnostic perspective to the neurobiological and neurophysiological basis of mental health (e.g. [5]), the development of disorder independent mental health assessment tools, such as the Mental Health Quotient, (see Assess your Mental Well Being) can offer a broader perspective to an individual’s mental health functions and concerns, without being constrained by arbitrarily defined disorder-based criteria.
References:
[1] Masi, A., DeMayo, M., Glozier, N., & Guastella, A. (2017). An Overview of Autism Spectrum Disorder, Heterogeneity and Treatment Options. Neuroscience Bulletin, 33(2), 183-193. doi: 10.1007/s12264-017-0100-y
[2] https://www.autismresearchcentre.com/arc_tests
[3] Goldani, A., Downs, S., Widjaja, F., Lawton, B., & Hendren, R. (2014). Biomarkers in Autism. Frontiers In Psychiatry, 5. doi: 10.3389/fpsyt.2014.00100
[4] Bosl, W., Tager-Flusberg, H., & Nelson, C. (2018). EEG Analytics for Early Detection of Autism Spectrum Disorder: A data-driven approach. Scientific Reports, 8(1). doi: 10.1038/s41598-018-24318-x
[5] Mitelman, S. (2019). Transdiagnostic neuroimaging in psychiatry: A review. Psychiatry Research, 277, 23-38. doi: 10.1016/j.psychres.2019.01.026


Hi Jennifer,
Thank you for both articles (2018 & 2019) on mental disorders. I was curious as to why you left out Simon Baron-Cohen and his lab. They have achieved some remarkable results in AS and autism assessment with their Empathy-Systemizing System (Baron-Cohen, The Empathizing System: A revision of the 1994 model of the mindreading system, 2005). Like me they have based their research on evolutionary psychology as this new science of the mind provides some helpful theoretical insights and a framework that is dearly missed in the more traditional psychology.
Hi Jan, Many thanks for your comment and insights into this topic. We’ve included a couple of Baron-Cohen measures in our review, but you’re right that we haven’t included those relating to the Empathy-Systemizing System. Thanks for pointing this out and we’ll make sure we include them as part of the wider research paper to see how they compare.
Hi Jennifer,
How much is asked of autistic people about their physical and energy experience – their physiology ? what it is like to live in their skin. Not about diseases, but about the ‘difficulty inside’ in relation to environments (people, living conditions, and own intense reactions).