Mental health is worst in young adults. How much worse and why? The Mental Health Million Project looks for insights.
Adolescence and young adulthood are considered to be the peak age range for the first onset of mental illness. Epidemiological data from the US, and globally, indicates that 75% of adults with a mental health disorder had experienced its onset by the age of 24 [1, 2], leading Thomas Insel, the former director of the National Institute of Mental Health (NIMH), to state that “Mental illnesses are the chronic diseases of the young.”[3]. What’s more, mental health difficulties in this younger age bracket seem to be increasing, as least in some places and for some subgroups. For example, a recent study in the US found that indicators of mood disorders and rates of deaths by suicide rose between the mid-2000s and 2017, primarily driven by increases among adolescents and adults aged 18 to 25 [4].
Mental Health across different age groups.
What we have seen from our initial data collection (~2400 individuals and counting), consistent to data reported elsewhere [5], is that younger adults report strikingly poorer mental health compared to older adults. In fact, our data show that there is a near linear relationship as you move up the age brackets from young to old (see figure below; data from first 1665 MHQ respondents). Across those in the 18-25 age bracket, the youngest age bracket we look at within the current project, nearly a quarter (23.7%) showed poor mental health that was at a Clinical or “At risk” level, in comparison to only 9.4% across the 65+ age group. The same picture plays out when you look at the percentage of young adults who have the mental capabilities needed to thrive or succeed in life – only 27% in young adults were Succeeding or Thriving compared to nearly 70% of those over the age of 65.
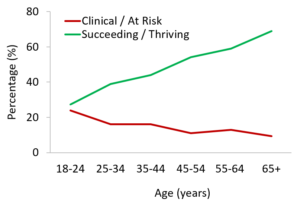
Percentage of respondents who were either Clinical/At risk (red line) or Succeeding/Thriving (green line) across different age brackets.
So why is this? What are the differences in the lives your younger adults, compared to older adults that are causing this considerable discrepancy in mental health?
Social Self as the key dimension of mental health challenges
The MHQ goes beyond an aggregate score to provide a view of six major categories of mental health. For example, the figure above shows the percentage of respondents (n=1665) who reported poor mental health that was at a Clinical or “At risk” level, for each of the 6 subcategories of mental health, across different age ranges. Social Self, which is a reflection of the perception of self relative to others, followed by Mood & Outlook are the ones with the highest percentage of people in the Clinical/At risk level, and this difference is most striking in early adulthood. This suggests that it is predominantly the emotional, social, and self-evaluative aspects of a young adult’s life which are negatively contributing to their poor mental health.
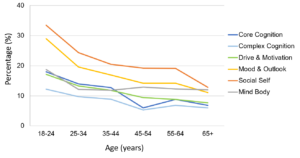
Percentage of respondents who were either Clinical/At risk in each of six subcategories of mental health
What is behind this? Is it to do with changing perception of oneself across the lifespan? Is it related to differences in usage and engagement with digital media and technologies? Could it be to do with differences in social contexts or adolescent experience? A changing social fabric? There are many possible explanations, and not only are there likely to be multiple underlying factors playing a role, but also the combination of these factors may differ across individuals, subgroups and geographies. Teasing apart the reasons behind these differences in mental health across age demographics, whilst also being able to compare across individuals, subgroups and geographies around the globe is one of the many objectives of the Mental Health Million Project.
The Mental Health Million Project
It’s discussions like these that motivated us to establish our Mental Health Million Project, which has an initial aim of mapping the mental health of 1 million individuals, young and old, across the globe. Over the past few months, we have been gathering data from individuals around the world, who have completed our online assessment called the Mental Health Quotient (MHQ) (https://sapienlabs.org/mhq/). This assessment allows individuals to gain an insight into their state of mental health and wellbeing, covers the broad spectrum of clinical symptoms through to mental assets and focuses on the consequences (good or bad) to an individual’s life.
Take part and help to build our understanding.
As the Mental Health Million Project progresses, we will be able to further explore how demographic factors, as well as other experiential, social, and situations factors, can influence mental health across different geographies, cultures and individuals. To help us reach our goal of 1 million responses, please take the MHQ and help us build our understanding of population mental health across the globe. Take it here: https://sapienlabs.org/mhq/
References:
[1] Kessler R, Bergland P, Demler O, et al. Lifetime prevalence and age-of onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry 2005; 62, 593-602
[2] Kessler, R. C., Amminger, G. P., Aguilar-Gaxiola, S., Alonso, J., Lee, S., & Ustün, T. B. (2007). Age of onset of mental disorders: a review of recent literature. Current opinion in psychiatry, 20(4), 359–364.
[3] Insel TR, Fenton WS. Psychiatric epidemiology: it’s not just about counting anymore. Arch Gen Psychiatry 2005; 62: 590-592
[4] Twenge, J. M., Cooper, A. B., Joiner, T. E., Duffy, M. E., & Binau, S. G. (2019). Age, period, and cohort trends in mood disorder indicators and suicide-related outcomes in a nationally representative dataset, 2005–2017. Journal of Abnormal Psychology, 128(3), 185–199.
[5] Substance Abuse and Mental Health Services Administration. Key substance use and mental health indicators in the United States: Results from the 2017 National Survey on Drug Use and Health (HHS Publication No. SMA 18-5068, NSDUH Series H-53). Rockville, MD: Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration; 2018. Retrieved from https://www.samhsa.gov/data/

